This activity for Diabetic Retinopathy education is provided by Med Learning Group.
This activity is supported by an independent medical education grant from Regeneron Pharmaceuticals, Inc.
Copyright © 2019Med Learning Group. Built by Divigner. All Rights Reserved.
Pathophysiology of PDR
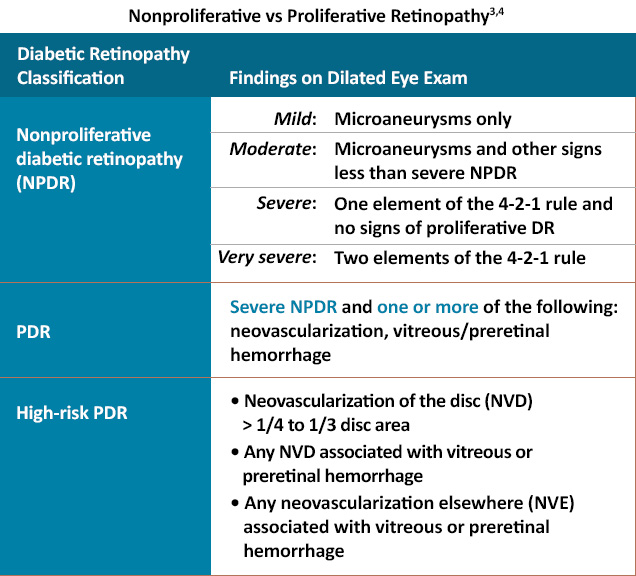
Diabetic retinopathy (DR) is a manifestation of end-organ ocular damage from systemic diabetes and chronically elevated blood glucose levels.1 While early stages of DR are typically classified as nonproliferative with varying stages of severity, proliferative diabetic retinopathy (PDR) develops as the disease progresses, often with significant visual consequences.1,2
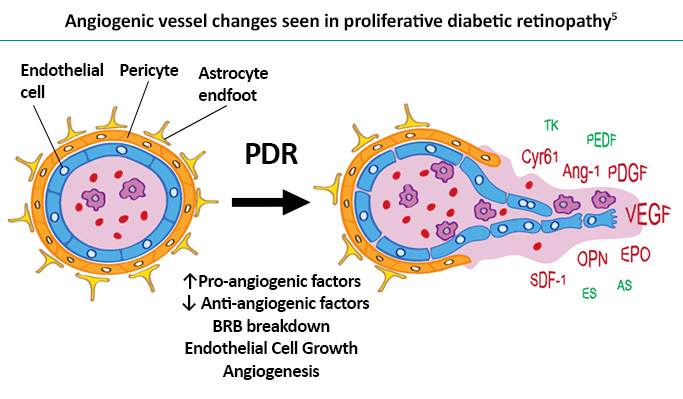
Chronic hyperglycemia from diabetes leads to tissue damage from various mechanisms, including microvascular damage, increased vascular permeability, inflammation, oxidative stress, and capillary occlusion.2 As capillary occlusion progresses, retinal hypoxia and ischemia worsen, triggering the upregulation of neovascular factors, including vascular endothelial growth factor (VEGF).2 VEGF perpetuates the damaging effects of diabetes by elevating local inflammatory factors, increasing vascular permeability, and promoting local inflammatory infiltrates.2
Increasing levels of VEGF from continued ischemia stimulates neovascularization to bypass occluded retinal vasculature. These new blood vessels originate from existing capillaries, mainly between perfused and non-perfused retina.2 However, neovascularization can also occur in the optic disc, iris, or filtration angle.1 Vessels from neovascularization are fragile, permeable, and bleed very easily, leading to complications like vitreous or preretinal hemorrhages, retinal detachments, and neovascular glaucoma.1
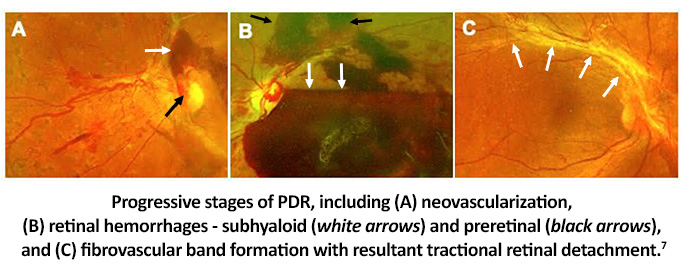
Neovascularization blood vessels can cross the retinal internal limiting membrane (ILM) into the vitreous cavity, using the posterior vitreous face as a scaffold.6 Not only do these vessels bleed easily, but they are often accompanied by fibrous proliferation.6 This fibrotic scar tissue sticks to the vitreous and ILM.6 The fibrous tissue can contract, pulling on the retina and leading to retinal vessel rupture and vitreous hemorrhage with or without tractional retinal detachment.6
Over time, chronic inflammation and vascular damage also lead to a breakdown in the blood-retina barrier and increased retinal vascular permeability.2,8 This ultimately results in fluid leaking into the tissues of the retina, especially under the macula, termed diabetic macular edema (DME).2
DME can be seen at any stage of DR and sometimes progresses independently of the other DR findings.3 The pathogenesis of DME is not well understood, but it likely involves all of the pathways previously mentioned, including angiogenesis, inflammation, and oxidative stress.8 Protein deposits from this edema lead to waxy, yellow findings referred to as hard exudates.2 DME is classified based on whether the edema involves the 1 mm center subfield zone.3

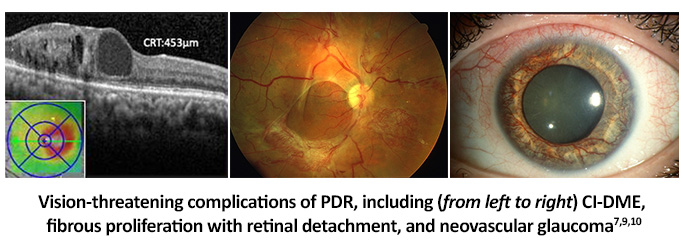
PDR is the most severe form of diabetic retinopathy, and vision loss can be exacerbated by CI-DME.1 Severe complications, such as vitreous or preretinal hemorrhages, retinal detachments, fibrosis, and neovascular glaucoma are consequences of PDR that can lead to significant visual impairment.1
References
- Flaxel CJ, Adelman RA, Bailey ST, et al. Diabetic Retinopathy Preferred Practice Pattern®. Ophthalmology. 2020;127:P66-P145
- Fontes ML, Falcao MF, Rosas V, et al. Diabetic Retinopathy Pathophysiology. EyeWiki. https://eyewiki.aao.org/Diabetic_Retinopathy_Pathophysiology
- Wong TY, Sun J, Kawasaki R, et al. Guidelines on Diabetic Eye Care: The International Council of Ophthalmology Recommendations for Screening, Follow-up, Referral, and Treatment Based on Resource Settings. Ophthalmology. 2018;125:1608-1622.
- Kim, JE, Feldman, JH, Shah, VA, et al. Diabetic Retinopathy. EyeWiki. https://eyewiki.aao.org/Diabetic_Retinopathy
- Abcouwer SF. Angiogenic factors and cytokines in diabetic retinopathy. J Clin Cell Immunol. 2013;Suppl 1:1-12.
- Mishra C, Tripathy K. Retinal Traction Detachment. StatPearls [Internet]. Last update February 21, 2022. https://www.ncbi.nlm.nih.gov/books/NBK558952/
- Cabrera AP, et al. Genotypes and phenotypes: A search for influential genes in diabetic retinopathy. Int J Mol Sci. 2020;21:2712.
- Kusuhara S, Fukushima Y, Ogura S, et al. Pathophysiology of diabetic retinopathy: The old and the new. Diabetes Metab J. 2018;42:364-376.
- Lewis K. Neovascularization of the iris (rubeosis iridis). Moran CORE. July 13, 2019. https://morancore.utah.edu/section-10-glaucoma/neovascularization-of-the-iris-rubeosis-iridis/
- Bozell C. Proliferative diabetic retinopathy (PDR) & tractional retinal detachment. Retina Imaging Bank. 2013;3494. https://imagebank.asrs.org/file/3494/proliferative-diabetic-retinopathy-pdr-traction-retinal-detachment
All URLs accessed 5/9/22.